Step 1. Identifying the Substitute Decision Maker
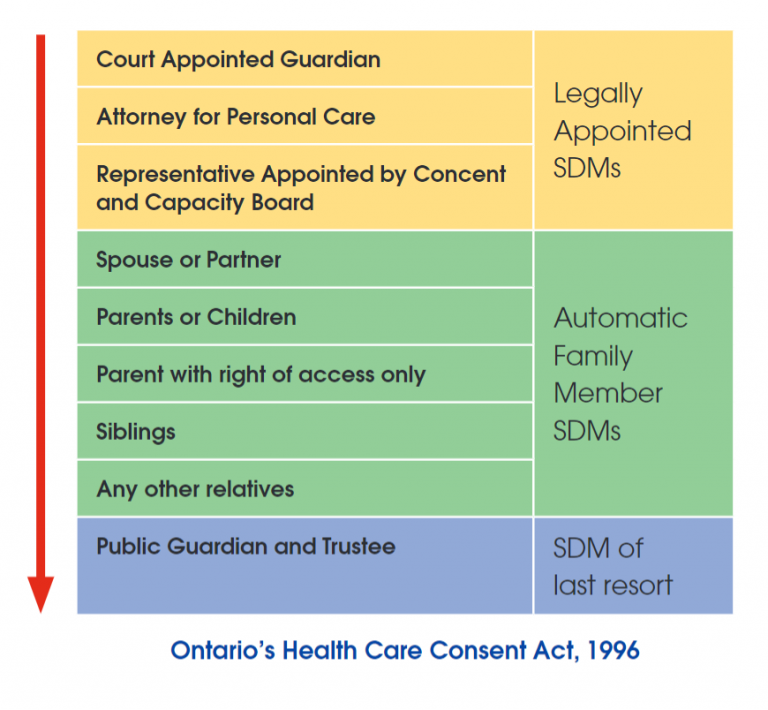
The first step is identifying the best Substitute Decision Maker (SDM). You can start off by asking your patients if they know who their SDM is. In Ontario, if someone hasn’t specifically appointed an SDM, then one of their family members would automatically become the SDM.
This is determined by a Substitute Decision Maker hierarchy where the highest-ranking person is a spouse or partner, followed by parents or children, parent with a right of access only, siblings, and then any other relatives.
You can advise your patients to:
- keep an Substitute Decision Maker wallet card in case of an emergency
- share who their SDM is with a few key people — this includes the SDM, a close family member and their primary health care provider
Power of Attorney for Personal Care (optional)
If a patient wants a different Substitute Decision Maker(s) other than the default person in the hierarchy, they must complete a document called a Power of Attorney for Personal Care. A Power of Attorney for personal care names a specific person or people as the Substitute Decision Maker(s).
The patient does not need a lawyer to prepare this document, and they can do it on their own if they are mentally capable. However, it needs to be witnessed by two people.

Step 2. Having conversations about your patients' values, wishes and beliefs
When talking to patients:
- focus on living well, not dying. Advance Care Planning is about quality of life.
- help them understand that having these conversations with their Substitute Decision Maker early and often is a gift.
- let them know their wishes can be shared orally, written down, or recorded on audio or video. It can be helpful for the Substitute Decision Maker to have a record of the conversation to return to if needed.

When the patient can no longer participate in healthcare decisions
If you’re supporting a person who can no longer participate in their healthcare decisions, encourage the Substitute Decision Maker to talk with the patient’s family and friends about what they know about the person’s values, wishes and beliefs and how this might guide personal care decisions.
“2/3 of patients have not spoken with their families about what's most important to them. ”